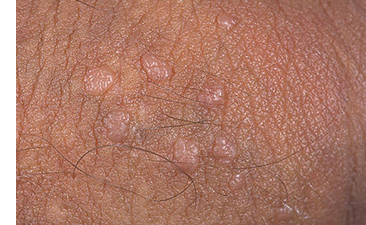 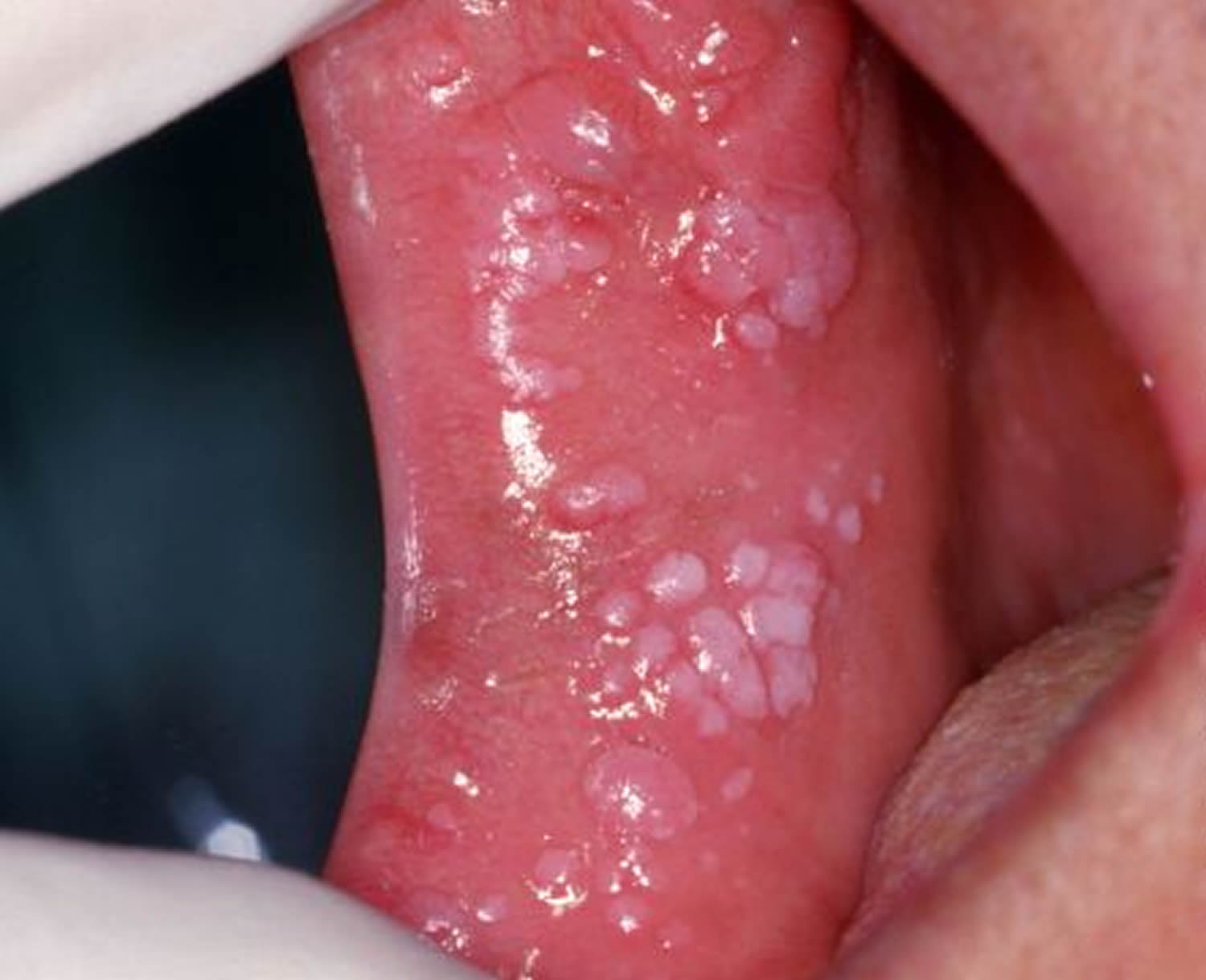
The HPV 9-valent vaccine, recombinant (Gardasil 9) can prevent HPV types 6, 11, 16, 18, 31, 33, 45, 52, and 58.The HPV quadrivalent vaccine (Gardasil) will protect against HPV types 6, 11, 16, and 18.The HPV bivalent vaccine (Cervarix) will only protect against HPV 16 and 18.The types of HPV the different vaccines protect against vary: Ask your doctor which vaccine they’re giving you People between the ages of 27 and 45 who haven’t been previously vaccinated for HPV are now eligible for Gardasil 9. The HPV vaccine involves two shots, separated by 6 to 12 months, for those ages 9 to 14 years.įor people ages 15 and over, three shots are given over six months. The HPV vaccine Gardasil 9 can protect against a number of types of HPV, including HPV 16 and HPV 18.įollow these tips to help prevent HPV: Get the HPV vaccination HPV 16 and HPV 18 are together responsible for approximately 70 percent of all cervical cancers worldwide. Like HPV 16, it doesn’t typically cause symptoms, but it can lead to cervical cancer. It causes 50 percent of cervical cancers worldwide. HPV 16 is the most common high-risk type of HPV and usually doesn’t result in any noticeable symptoms, even though it can bring about cervical changes. You can apply these medications directly to your genital warts. This local destruction of the wart tissue helps enhance your immune system’s ability to fight the STI virus. These are topical medications that destroy genital wart tissue. If you do contract HPV 6 or HPV 11, your doctor can prescribe medications such as imiquimod (Aldara, Zyclara) or podofilox (Condylox). The recommendation is to receive the vaccines prior to becoming sexually active, since the vaccine can’t protect against a strain of HPV that a person has already been exposed to. This significant reduction against contracting these types was noted in 9- to 26-year-olds. The vaccine also offers some protection from HPV 11.įor the HPV vaccine Gardasil 9, clinical trials showed up to 89 to 99 percent effectiveness in protecting against HPV types 6 and 11. Getting the HPV vaccine may help prevent HPV 6. They usually show up a few weeks or months after exposure from a sexual partner who has HPV. Genital warts look like cauliflower-shaped bumps on your genitalia. HPV 11 can also cause changes to the cervix. They are linked to approximately 90 percent of genital warts. HPV 6 and HPV 11 are low-risk types of HPV. Your doctor will monitor your condition so that if cancer cells do develop, they can be detected early. Some types of HPV clear up without intervention. The cost per successful treatment course is approximately $200 to $300 for podofilox, cryotherapy, electrodesiccation, surgical excision, laser treatment, and the loop electrosurgical excision procedure.If you’ve contracted HPV, identifying the type you have helps your doctor determine next steps. Fluorouracil and interferon are no longer recommended for routine use. Podofilox, imiquimod, surgical excision, and cryotherapy are the most convenient and effective options. Patient-applied therapy such as imiquimod cream or podofilox is increasingly recommended. The choice of therapy is based on the number, size, site, and morphology of lesions, as well as patient preferences, cost, convenience, adverse effects, and clinician experience. 
The goal of treatment is clearance of visible warts some evidence exists that treatment reduces infectivity, but there is no evidence that treatment reduces the incidence of cervical and genital cancer. Biopsy, viral typing, acetowhite staining, and other diagnostic measures are not routinely required. Evidence guiding treatment selection is limited, but treatment guidelines recently have changed. Genital warts caused by human papillomavirus infection are encountered commonly in primary care.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
